Pitfalls in the Diagnosis of Skeletal Tuberculosis in Children
Janani Sankar 1*, Sriram N1, Supreetha Shetty 1
1 Department of Pediatrics & Pediatric Orthopedics, Kanchi kamakoti childs trust hospital, Chennai, India.
*Correspondence Author:Janani Sankar, Senior Consltant, Pediatrics, Department of Pediatrics & Pediatric Orthopedics, Kanchi kamakoti childs trust hospital, Chennai, India, Tel: +91 44 4200 1800; Fax: +91 44 4200 1800; E-mail: janani.sankar@yahoo.com
Citation:Janani Sankar, Sriram N, Supreetha Shetty (2022) Pitfalls in the Diagnosis of Skeletal Tuberculosis in Children. Pediatr Primary Physic 2:107.
Copyright: © 2022 Janani Sankar, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Received date: November 19, 2022; Accepted date: December 11, 2022; Published date: December 14, 2022
Abstract
Skeletal tuberculosis in children can easily be missed due to their non specific presentations. The objective of our study is to review the varied presentation, pitfalls in the diagnosis of pediatric skeletal tuberculosis and treatment outcome. A retrospective review of children diagnosed with skeletal tuberculosis over a period of 3 years. A total of 19 cases were reviewed. Mean age was 5.6 years. Average duration of symptoms was 6 months with chronic pain being the most common. spine was the commonest site. Most of the cases were missed due to non specific presentation, hence delaying the diagnosis. Contact history was positive in 6 and ESR was elevated in majority of them. Diagnosis was confirmed radiologically, bacteriologically or histopathologically. All children were treated with anti tubercular drugs and surgical debridement with good prognosis. A high index of suspicion aided by confirmation using imaging or histopathology can help in early diagnosis. Treatment with anti tubercular drugs with surgical debridement has good prognosis.
Introduction
Skeletal tuberculosis refers to involvement of bone and joints. It is an ancient disease and the features of spinal tuberculosis has been identified in Egyptian mummies dating back to 9000 BC.
Skeletal tuberculosis accounts for 5-8% of extrapulmonary tuberculosis. It can present with a broad spectrum of variable clinical manifestations which can cause diagnostic difficulties. There is often a delay in diagnosis of pediatric skeletal tuberculosis due to its non specific presentation. To further elucidate the possible diagnostic pitfalls 19 cases of radiologically, bacteriologically and histopathologically proven cases of pediatric skeletal tuberculosis are reviewed, some of which were initially diagnosed otherwise. We intend to highlight few cases where the diagnosis was missed initially and consequently treatment was delayed. We would like to discuss in this case series the various modes of presentation, diagnostic modalities and treatment.
Materials and Methods
All the children who were diagnosed with skeletal tuberculosis from the year 2012 to mid 2015 and treated at Kanchi Kamakoti CHILDS trust hospital, chennai were retrospectively reviewed. Their clinical details, laboratory data, imaging modalities and histopathology reports were analysed. The age group affected, sex predominance , time lag between the onset of symptoms to the diagnosis of the disease , site involved, inflammatory markers, contact history, status of BCG immunization (based on scar and history), treatment modalities (surgical and chemotherapy) and prognosis at the completion of treatment were also studied. Few interesting cases which were treated otherwise initially are also highlighted.
Results
A total of 19 cases of pediatric skeletal tuberculosis in a duration of three and a half years (2012 to mid 2015) were reviewed. Diagnosis was based on radiolography, bacteriological examination and histopathology. There were 12 female and 7 male children in our study with a female predominance constituting 63.16%. The mean age of affected children was 6 years with the youngest being 13 months and the oldest 13 years of age.
Tuberculosis of spine constituted the maximum number accounting for 52.63% of the cases among which 77.77% involved the thoracic vertebrae followed by lumbar and thoraco-lumbar vertebrae constituting 11.11% each. The next most common sites to be involved were hip and the knee joint each of which accounted for 15.79%. There was one case each of tuberculosis of the shoulder joint and the phalanx.
The average duration of symptoms prior to diagnosis was five and a half months with the earliest being diagnosed at 1 month and the latest at 2 years after the onset of symptoms. It was noted that pain was a consistent symptom in all the cases. Pain at the site of the lesion was the most common presenting symptom and was present in 17 patients which constituted to about 89.47% of cases. Referred pain was present in the remaining 2 cases. Other presenting symptoms were restriction in the range of movements of the involved part in 47.37% followed by obvious swelling or deformity at the site which was present in 42.11% cases. Weight loss was present in 26.32% cases. Interestingly fever was present only in 4 children (21.05%). Loss of appetite and reduced activity were present in 10.53%.
Contact history was positive in 6 children (31.58%). BCG scar was absent in 2 children (10.52%) and was consistent with history of incomplete immunization status. Mantoux test was noted to be positive in 3 of them which constitutes to 15.79%.
ESR was done in all cases. Significant increase in ESR (>50mm/hr) was noted in 66.66%. Mean ESR was 61mm/hr with highest being 100 mm/hr.
In terms of imaging studies, the most consistent finding was osteolytic lesion on plain radiography and MRI which was present in all cases. Cold abscess in MRI was noted in 33.33%. Periarticular soft tissue edema was present in 22.22%. Given the high possibility of tuberculosis infection in our country it was strongly considered as a diagnosis with the above findings in children where there was a high index of suspicion. Chest X-ray was done in all cases and no pulmonary involvement was found in any of them. Extraskletal manifestation was present in one child in the form of tuberculous lymphadenitis.
Histopathology was suggestive of tuberculosis in 15 children (78.95%). Culture was positive in 1 child, PCR for tuberculosis was positive in 1 child and the remaining 2 were diagnosed radiologically. All the children received both surgical as well as medical treatment. Surgical debridement with stabilization of the part involved was achieved in all of them. Treatment with four antitubercular drugs (rifampicin, isoniazid, streptomycin, ethambutol) for a total period of 9 months was instituted in all 19 children.
At follow up after 6 months of starting treatment and after completion of ATT the outcome was good. In children who have completed their course of treatment as of now, full range of movements with no residual deformity and complete radiological resolution was noted.
Discussion
Despite a global reduction in tuberculosis, extrapulmonary tuberculosis is on the rise. A recent global resurgence of tuberculosis resulted in the United Nation’s millennium development goal 6 targeting halving the tuberculosis prevalence and mortality rates of 1990 by 2015. Although this target is on track, extrapulmonary tuberculosis which is diagnostically more difficult is showing a relative increase [1,2]. As per WHO report of 2014 an estimated 550000 children became ill with tuberculosis and 80,000 HIV negative children died of tuberculosis in 2013. One fourth of all tuberculosis cases are in India [3].
To facilitate the early diagnosis of skeletal TB and to avoid the possibility of complications in the management of patients, medical practitioners should be familiar with the usual forms of presentation of the disease and the wide variety of clinical manifestations. Presently diagnostic modalities have improved. Diagnostic facilities like imaging (ultrasonography, plain radiograph, MRI), USG guided aspiration of synovial fluid for XPert TB and HPE must be utilized.
In our case series we studied a total of 19 cases of skeletal tuberculosis with respect to age, sex, mode of presentation, site and time lag in diagnosis from 2012 to mid 2015. Extrapulmonary tuberculosis was found to constitute 68.5% of all TB cases during the period with skeletal TB among these constituting 30%. This was much higher than the reported incidence of 5-6% [4]. We found a higher incidence of the disease in female children when compared to male children.
The most common presenting symptom in our case series was pain followed by restriction in range of movements of the part involved and swelling or deformity at the site. This is consistent with the study done by Harish.S.Hosalkar et al. on skeletal tuberculosis in children [5]. Systemic symptoms were interestingly rare in the children reviewed. Due to the non specific presentation and the chronicity of symptoms various differential diagnoses should be considered. However tuberculosis should be suspected in all children with complaints of chronic bone pain with or without deformities even in the absence of systemic symptoms. Skeletal tuberculosis is not life threatening and can be treated if diagnosed early before bone destruction ensues.
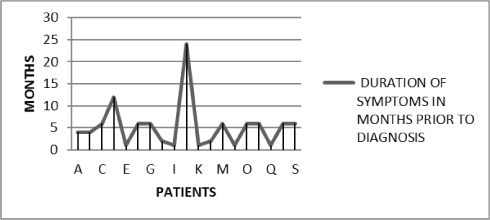
The mean duration from the onset of symptoms to diagnosis was found to be five and a half years with the most delayed diagnosis being after 2 years of starting of symptoms. We noticed that the children diagnosed late were the ones with non-specific symptoms and presentation [Figure 1].
The youngest child in our case series was a 13 month female child with spina ventosa. She presented with a swelling and redness of left index finger of one month duration. A differential diagnosis of enchondroma was considered initially. MRI however was suggestive of infection. She underwent curettage and bone grafting. The histopathology was diagnostic of tuberculosis.
The longest duration of symptoms in our case series was 2 years in three and a half years female child with tuberculosis of the thoracic spine. She had complaints of torticollis of 2 years duration. Imaging of the spine was suggestive of tuberculosis and was proven by histopathology.
Contact history was present in 31.58% of our cases. Similar incidence was noted by Vijayasekaran et al. who studied the contact positivity in pediatric tuberculosis [6]. Contact history can prove to be useful in unusual presentations suggesting otherwise as in one of our cases and can help pick up cases early.
ESR was elevated in majority of our cases and may be an important marker. Plain radiograph is a cost effective initial investigation. In our case series all the children had osteolytic changes on plain radiographs. It has been reported that only 3-6% patients with bone, joint or spinal tuberculosis have normal plain radiographs [7]. MRI is also a very informative imaging modality and helps to know the extent of skeletal involvement.
The gold standard for diagnosis is histopathological confirmation of a tissue sample. Tuberculous granulomas with multinucleated giant cells, epitheloid histiocytes, lymphocytes and plasma cells can be seen in the tissue sample.
Cultures in skeletal tuberculosis are seldom positive and in our study we had one child with culture proven tuberculosis. This is usually because the organism needs to be in specific conditions to be cultures and a longer incubation period is required for in vitro growth [8].
The treatment of skeletal tuberculosis includes administration of anti tuberculous drugs. Few authors suggests that medical treatment alone is sufficient while others argue that surgical debridement and drainage is required [7]. In our case series all the children underwent debridement with stabilization. ATT with 4 drugs was administered for a period of 9 months. With the above management on follow up after completion of treatment all children who have completed their treatment as of now were noted to have full range of movements with no residual deformities.
Conclusion
Skeletal tuberculosis not a rare disease and is very much amongst us. To make an accurate and early diagnosis medical practitioners should be aware that it can simply present as chronic pain with no other clues in children. High index of suspicion in an otherwise healthy child presenting with the above discussed non specific symptoms can help in making an early diagnosis and institution of treatment. Laboratory parameters, skeletal imaging, bacteriology and histopathology are of importance in confirming the diagnosis. Prompt treatment can reduce the morbidity and mortality associated with the disease.
References
- The WHO Millenium Development Goals Report. 2013
- Te Beek LA, van der Werf MJ, Richter C, Borgdorff MW (2006) Extrapulmonary tuberculosis by nationality, The Netherlands, 1993-2001. Emerg Infect Dis 12: 1375-1382. [crossref]
- Global Tuberculosis Report 2013; Executive Summary, WHO/HTM/TB/2013.15.pp2
- Powell DA, Hunt WG (2006) Tuberculosis in children: an update. Adv Pediatr 53: 279-322. [crossref]
- Hosalkar HS, Agrawal N, Reddy S, Sehgal K, Fox EJ, et al. (2009) Skeletal tuberculosis in children in the Western world: 18 new cases with a review of the literature. J Child Orthop 3: 319-324. [crossref]
- Vijayasekaran D, Kumar RA, Gowrishankar NC, Nedunchelian K, Sethuraman S (2006) Mantoux and contact positivity in tuberculosis. Indian J Pediatr 73: 989-993. [crossref]
- Monach PA, Daily JP, Rodriguez-Herrera G, Solomon DH (2003) Tuberculous osteomyelitis presenting as shoulder pain. J Rheu-matol 30: 851–856.
- Watts HG, Lifeso RM (1996) Tuberculosis of bones and joints. J Bone Joint Surg Am 78: 288-298. [crossref]
