An eICU/ICU Collaborative to Reduce Sepsis Mortality
Laura Maples1*
1 University of San Francisco, California, USA.
*Corresponding Author: Laura Maples, University of San Francisco, California, USA, TEL:(415) 422-6525 ; FAX:(415) 422-2677 ;E-mail:lmaplesrn@gmail.com
Citation: Laura Maples (2019) An eICU/ICU Collaborative to Reduce Sepsis Mortality. Arch Mol Med & Gen 1:108.
Copyright: : © 2019 Laura Maples, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Received date: January 09, 2019; Accepted date: February 28, 2019; Published date: March 04, 2019.
Abstract
Sepsis costs over 20 billion dollars annually to treat making it the most expensive diagnosis for hospitals [1] and carries with it an average mortality rate of 45% [2]. The eICU/ICU collaborative project was developed to improve sepsis mortality at Sutter Health’s Solano hospital affiliate from 41.2% to the system-wide goal of 18.8% over the course of a year by implementing two technologies. The first was the onboarding of the non-invasive cardiac output monitoring (NICOM) technology by Sutter Solano to fulfill the 6-hour bundle compliance for septic shock resuscitation. The other technology was the activation and enhancement of the Core Measure Manager (CMM) high-quality data surveillance technology by Sutter’s eICU to screen all patients at Sutter Solano Medical Center for early identification and treatment of sepsis and septic shock. After twelve months of quality improvement measures including education, training, implementation, enhancement, tracking and treatment management; the dashboards revealed Sutter Solano’s sepsis/septic shock mortality rate dropped from 41.2% to 6.1%. Nurses and physicians need to recognize that central venous pressure (CVP) is no longer a recommended or accepted measure of hemodynamic stability. The latest evidence-based practice supports NICOM in conjunction with passive leg raise (PLR) as a foundational guideline for fluid resuscitation. The Clinical Nurse Leader (CNL), as systems analyst and risk anticipator, must manage information as well as the care environment to improve quality patient outcomes in the presence of evolving knowledge and the ever-changing healthcare system [3].
Keywords
eICU, telemedicine, interdisciplinary collaboration, quality improvement, hemodynamic monitoring, high-quality data surveillance, NiCOM, vasopressors, sepsis/septic shock, mortality, early goal-directed therapy (EGDT), fluid resuscitation.
Introduction
The diagnosis of Sepsis or Septic Shock carries with it a high mortality rate as well as high costs to patients and the systems which provide the care these patients need. Klompas and Rhee [4], with grant funding support from the Centers for Disease Control (CDC), performed a research into sepsis surveillance. They support the early identification and treatment of sepsis which continues to evolve with technology and information systems. The teams which deliver this care must accommodate the latest evidence-based practice (EBP) to provide the best possible outcomes for their patients. The Clinical Nurse Leader (CNL), as systems analyst and risk anticipator, must manage information as well as the care environment to improve quality patient outcomes in the presence of evolving knowledge and the ever-changing healthcare system. The following is an account of the collaborative clinical outcomes management of septic patients at Sutter Solano Medical Center.
The electronic-intensive care unit/ intensive care unit (eICU/ICU) collaborative project aims to improve sepsis mortality outcomes at Sutter Solano. The project began on June 1, 2016 with an ICU/eICU collaborative for quality improvement. The project ends May 1, 2017, with the roll-out of the April 2017 benchmark reports or when the sepsis mortality reaches 18.8%, the organizational target. By working on this process, the team expects to decrease mortality rates for septic patients from 41.2% to 18.8%. It is important to do this work now to save patient’s lives, to improve their long-term outcomes and to reduce cost burdens of hospitalization and self-care management.
The project is an evidence-based activity that plans to improve performance, delivery and quality of care. It involves implementation of established and tested quality standards for hemodynamic monitoring as well as enhancing and implementing existing high quality data surveillance technologies. The project provides performance measures to ensure compliance with existing quality standards, care practices and interventions. Further this project received no funding from federal agencies or research organizations. All Sutter Health names and information were used with permission from Sutter Health’s quality documentation and quality risk managers.
Clinical Leadership Theme
The CNL theme involved in this project is consistent with organizational and systems leadership. This project required the CNL to assume a leadership role within the interprofessional team using effective communication to successfully implement a collaborative patient safety and quality improvement initiative [3]. The first aspect of the collaborative requires that Sutter Solano Medical Center on-board a non-invasive cardiac output monitoring (NICOM) device to determine fluid responsiveness and better guide therapies in their septic patients. Because the eICU is integral in the critical care management of these patients, the CNL must laterally integrate and coordinate the education of the eICU staff to the NICOM equipment. Further, as a liaison between members of a health care team, the CNL will ensure lateral partnering with the bedside quality improvement team consisting of nurses, physicians, pharmacists and laboratory personnel to manage necessary early treatment in this vulnerable patient population.
The CNL leadership theme [5] also pertains to being an information manager utilizing information systems and technology at the point of care to improve patient outcomes. The CNL will partner with eICU management, pharmacy and electronic health record (EHR) personnel to evaluate the impact of the new high-quality data surveillance core measure manager technology (CMM) on patient outcomes. Together they will manage the information to continually improve and enhance this technology to its effective and meaningful use.
Statement of the Problem
The problem occurred as the mortality outcomes for septic patients at Sutter Solano rose to 41.2%, well over the national average of approximately 28.8% and the system-wide threshold of 18.8%. The query is whether the incorporation of hemodynamic monitoring for fluid responsiveness and the use of high-quality data surveillance can improve the mortality rate to the system-wide threshold of 18.8%. Careful consideration for the impact of the eICU/ICU collaborative effort is required to effectively evaluate this project. The hands-on care is provided by Sutter Solano’s critical care and emergency room nurses and hospitalists while the remotely located eICU expert critical care nurses and intensivists manage these critically ill patients during off-hours. Further, the high-quality data surveillance CMM technology which screens all of Sutter Solano’s patients for sepsis, is managed by the eICU nursing team.
Rationale
According to the Society of Critical Care Medicine [2], 20% of the annual 5.7 million patients admitted to hospitals go to an intensive care unit. Additionally, 58% of emergency room admissions result in an ICU admission. Sepsis is the second leading cause of death in non-coronary ICUs with a mortality rate of up to 45%. Afrefian, et al., [1] tell us that hospitals spend over 20 billion dollars annually to treat sepsis making it the most expensive diagnosis to treat. What stakeholders need to know is that $1 billion per quality life year gained can be saved through quality critical care management of severe sepsis, acute respiratory failure and general critical care interventions [2]. Critical Care management, which is provided by the eICU on average16 hours/day, consists of early recognition; timely, appropriate and consistent treatment; and the provision of expert guidance for emergent interventions. It must also be consistent with the latest EBP. This project explores the latest EBP and the variance from the treatment that has guided septic shock resuscitation for the last twelve years as a potential for improvement in quality outcomes for septic patients.
Project Overview
A project analysis revealed a pattern of increasing mortality for septic patients at Sutter Solano Medical Center. The purpose of the eICU is to improve patient quality outcomes through increased collaboration and through provision of board certified intensivist and expert critical care nurses and staff. The process analysis during the rolling months of February-April 2016, revealed Sutter Solano had a severe sepsis/septic shock mortality rate of 41.2%, well above the national average of 14.7 to 29.9% [6]. Solano’s data revealed greater than 85% compliance with 3-hour bundles: measuring a lactate level; drawing blood culture; giving the antibiotic within an hour of a sepsis alert/diagnosis; and adequate fluid resuscitation. They also provided vasopressors appropriately. Their compliance decreased to 77.3% for remeasuring lactate levels greater 2.0. Additionally, they had virtually no means of hemodynamic monitoring and only performed the 6-hour bundle element of a focused physical exam 42.9% of the time.
The discovered need was for improved capture, follow-up and management of this vulnerable patient population. To accomplish improved sepsis mortality outcomes from 41.2% to the organizational threshold of 18.8% by May 1, 2017, the eICU/ICU collaborative initiative was activated. Quality improvement teams, unit champions and leadership from both Solano’s ICU and the eICU began analyzing and communicating regarding avenues for quality improvement measures in collaborative effort to improve these outcomes.
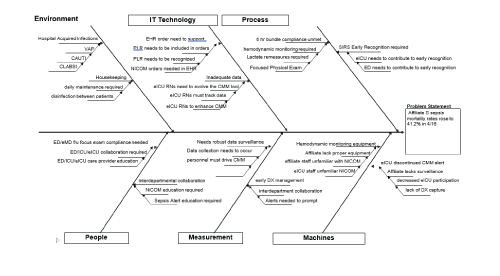
Potential problems anticipated in this project included access to equipment. Mitigating the impact required to expedite NICOM equipment purchases was achieved by the affiliate early in the initiative timeline. High-quality data surveillance was required to screen all inpatients. This required working with the EHR team and the pharmacy administration to incorporate smart alerts that would screen for signs and symptoms of sepsis. The progression of this process required frequent reconfiguring of the smart alert. Its evolution is ongoing and feedback dependent. The CMM program is a sensitive marker that grows more specific with each restructured iteration (see “RCA Fishbone Diagram” Figure 1).
Cost Analysis
There is a reasonable business case for the eICU/ICU collaborative project to reduce sepsis mortality at Sutter Solano Medical Center from 41.2% to the system-wide benchmark of 18.8%. The costs for this project include 400 student practicum hours at hypothetical $65.00/h for a total of $26,000.00, and the purchase and adoption of two new technologies. Three NICOM machines, at $10,000.00 each, totaled $30,000.00. Bedside staff training costs are to be determined (TBD) but estimated at less than $10,000.00. The eICU training sessions/presentations costs for 15 staff at $65.00/hr totaled $975.00. Other pharmacy and leadership change agents collaborated to enhance and implement the CMM program alert technology during time already spent productively. Total costs equaled @ $66,975.00.
Savings are reflected in sepsis mortality rates dropping from 41.2% in April 2016, to 6.1% in March 2017, a 68% decrease. Benefits to the Sutter Health System can be calculated in lives saved through the eICU/ICU collaborative efforts from June 2016, through April 2017. In 2017, ten lives were saved that were not expected to survive. The Society of Critical Care Medicine [2] states critical care management of sepsis, including acute respiratory failure saved $1 billion per quality life year gained in 2005, before today’s soaring healthcare prices. Additionally, the qualitative benefits provided by this project impact improved sepsis mortality rates at Sutter Solano and improved quality of life for those patients surviving sepsis. The primary key stakeholders of this project are the patients diagnosed with sepsis and septic shock. As other key stakeholders, the system administrators and leadership are encouraged to decrease mortality rates and improve outcomes. Further stakeholders include those persons and entities who provide education and presentations on new technologies as well as the healthcare educators. Others still are those staff who provide care to this population which include unit champions from eICU, ICU, ED, laboratory, pharmacy, EHR and medical physician champions. Each invested their time to ensure the implementation and activation of the various cycles of change involved in the onboarding of the NICOM and CMM technologies. These team members continue to participate in the early identification and treatment as well as the critical care management of these patients when they respond to sepsis alerts and apply the skills required to manage septic shock resuscitation. Through the application of these quality improvement measures, these staff significantly improve outcomes for septic patients (see “Cost Analysis” Figure 2).

Methodology
This change project began in June 2016, and was favored with strong characteristics for successful innovation diffusion. According to Massoud, et al., [7], these characteristics are: relative advantage; trialability; observability; communications channels; homophilous groups; pace of innovation/reinvention; norms, roles, and social networks; opinion leader; compatibility; and infrastructure. The change was facilitated by strengths in all these factors. Challenges existed only to the extent that the group was not homophilous and that staff opinion leaders were sometimes the slower adopters. Infrastructure required adoption of the new NICOM technology and development and enhancement of the CMM technology. A particularly strong innovation characteristic was founded in the eICU’s simultaneous pursuit of the American Association of Critical-care Nurses’ (AACN) Beacon Award which directed the unit’s attention to internal quality improvement. However, this quality improvement project was more accurately guided by Kotter’s [8] eight steps to change for transformational leadership. These steps are: to establish a sense of urgency; create a powerful guiding coalition; develop a vision; communicate the vision; empower others to act; plan for and create short-term wins; consolidate improvements for more change; and institutionalize new approaches.
A sense of urgency rose when the system-wide benchmark report statistics were shared during the eICU Partnership Council (PC). Increasing sepsis mortality rates at Sutter Solano Medical Center inspired an eICU change agent, a Solano ICU Unit Champion RN, and an eICU Unit Champion, who was also the CNL student, to propose a “Sutter President’s Award Collaboration”. This shared vision would drastically improve sepsis mortality outcomes by bridging interdepartmental efforts and resources. The Solano bedside ICU and Emergency Department (ED) team adopted and implemented hemodynamic monitoring. The eICU implemented high quality data surveillance to identify patients with and at risk for sepsis throughout Sutter Solano. The eICU team, in conjunction with the bedside care providers, then managed the NICOM in-time critical care interventions during off-hours.
The eICU team communicated the vision through multiple hemodynamic monitoring presentations and eICU Journal Club explorations in the latest EBP for fluid responsiveness. Additionally, the daily knowledgeable, successful and well-directed in-time interventions with Solano’s septic patients empowered the eICU and ICU staff to act on the vision with regularity.
The high-quality data surveillance CMM program which monitors Sutter Solano for septic patients also provides information which was used to modify and improve the tool. Regular updates on Solano’s mortality rates were reported during monthly Beacon and PC meetings revealing continued improvement. Wins were reported as lives saved at Sutter Solano. The potential spread of the CMM high-quality data surveillance technology to other affiliates could be determined based on benchmark results in May 2017.
This eICU/ICU collaborative to reduce sepsis mortality at Sutter Solano Medical Center is a two-armed project. The bedside team adopted and implemented hemodynamic monitoring equipment on all patients with a diagnosis of septic shock. The NICOM was used to determine fluid responsiveness and resuscitation strategies rather than relying on the previous standard central venous pressure (CVP) reading. Simultaneously, the eICU employed at Solano an enhanced CMM technology for high quality data surveillance screening for sepsis on all emergency room and inpatients. Both units have overcome barriers and undergone nine months of PDSA cycles that have included technology and equipment education and implementation, use of screening tools and checklists and the creation of excel databases for monitoring quality interventions (see “SWOT Analysis” Table 1).
Table 1: SWOT Analysis.
| Strengths: 1.eICU Leadership is very supportive. 2.ICU leadership is very supportive. 3.Unit Champions from both sides are collaborative. 4.ICU leadership readily purchases NiCOM equipment. 5.Project contains strong diffusion innovation factors. |
Weaknesses: 1.Knowledge level requires exposure and education. 2.Opinion leaders require recruitment. 3.Strength of initiative requires. 4.Collaboration between involved units and departments required. 5.CMM monitoring is an additional responsibility/duty to eRN workflow |
| Opportunities: 1.Sepsis mortality rates could improve from 41.2% to system benchmark of 18.8%. 2.Initiative improvements could lead a system-wide improvement cycle. 3.Enhanced CMM technology could benefit system. 4.Instituting NiCOM technologies could lead industry towards best EBP. |
Threats: 1.NiCOM use requires standardized mechanism PLR to be consistent. 2.Old information and knowledge currently guide care. 3.Familiar practices of CVP measurements are obstacles to incorporating new ideologies. 4.Adequate staffing is required for adequate data surveillance. |
Marx and Scheeren [9] argue that while hemodynamic monitoring is the foundation for determination of fluid responsiveness, CVP measures are static and therefore should not be used to gather this information. They contend that these critically ill patients need physicians to use hemodynamic monitoring equipment regardless of their familiarity with it as their knowledge will grow with experience. Sutter Solano and eICU physicians who have exposure to the latest EBP and NICOM technology information have been eager and willing to incorporate the change.
The desired goal of the collaborative project would be reached when patients diagnosed with sepsis and septic shock at Sutter Solano Medical Center experience improved mortality rates from 41.2% last year to a goal of 18.8%. These results exceeded expectations when the mortality rate at Solano in March 2017, had already decreased to 6.1% through these interventions. This goal was accomplished through hemodynamic monitoring to determine septic shock decision tree interventions such as fluid resuscitation and use of vasopressors. A CMM high quality data surveillance alert system was implemented and enhanced by the eICU to screen all patients at Sutter Solano for sepsis and septic shock. The quality data report for April of 2017, revealed results from the clinical interventions. A comparison of this data to last year’s data determined this collaborative project was effective. Skeptics of the project expressed that the improved results were a product of the CMM capturing more, less intensively ill patients, driving decreasing mortality rates by less severity. In fact, the prior 11 months to the incorporation of the CMM technology had an average monthly denominator of 13.0 patients. The later 11 months had an average denominator of 10.36 patients. After subtracting the single outlying denominator of 18 from the prior 11 months, the average monthly denominator before CMM activation was 10.1 patients. This variance is insignificant to drive the data’s considerable change in results.
Data Source/Literature Review
The search statement that drove this project’s literature review follows: Will hemodynamic monitoring for fluid responsiveness and high quality data surveillance improve the mortality rate outcomes for septic patients at Sutter Solano Medical center from a prior 41.2% to the system-wide threshold of 18.8%? The search statement explores the population, intervention, comparison, outcome and timeframe (PICOT) of a change project. The population is that of all septic patients at Solano. The interventions consist of a two-pronged collaborative effort use of NICOM and CMM technologies. The comparison is between sepsis mortality data from April 2016, to sepsis mortality data gathered until March 2017. The expected outcome was a decrease in sepsis mortality at Sutter Solano from 41.2% to 18.8%.
The search through CINHAL, SCOPUS and PubMed databases using Boolean phrases of ‘sepsis’ and ‘ICU’ in different combinations, with limits of peer reviewed articles and EBP in the last five years revealed 27 articles, 9 of which are relevant. The search for Boolean phrases of ‘hemodynamic’ ‘monitoring’ and ‘sepsis’ revealed 121 articles, most were older than five years and many others were outdated by new criteria for defining sepsis. Included is one article from 2001 which defined early septic shock treatment modalities and multiple other articles that argue for and explain hemodynamic monitoring through impedance and bioreactance processes.
The search through CINHAL, SCOPUS and PubMed databases listed over 2000 articles on high quality data surveillance. When including “Sepsis” in the Boolean phrase, only 200 articles appeared, six of which were pertinent to this project because of their instruction and evaluation of efficacy and sensitivity to screening for sepsis. Based on these literature review, research explaining hemodynamic monitoring evidence and high-quality data surveillance will be reviewed.
Hemodynamic Monitoring Evidence
Rivers, et al, [10] performed a prospective, randomized control study involving 263 participants diagnosed with severe sepsis and septic shock. Their article provides standard definitions for systemic inflammatory response syndrome, (SIRS), severe sepsis and septic shock that continue to guide care for this vulnerable population today. SIRS was defined as the presence of infection with two or more of the following associated symptoms: temperature >/= 38°C or 90/minute; respiratory rate > 20/minute or pCO2 < 32 mm Hg; and white-cell count >12.0 or < 4.0. Severe sepsis was defined as SIRS with added end-organ dysfunction/failure as indicated by: systolic blood pressure 2.0; creatinine > 2.0; Bilirubin > 2.0; urinary output, 0.5ml/kg/hr for >2 hrs; or mean arterial pressure (MAP) < 70 mm Hg. Septic Shock was defined as severe sepsis with lactate >4 or the requirement of a vasopressor after the initial crystalloid fluid resuscitation of 20-30 ml/kg over 30 minutes.
Rivers, et al, [10] used the septic shock definitions as the inclusion criteria for their study. Early goal-directed therapy (EGDT) was randomly provided to 130 participants and 133 received standard care. EGDT provided multiple treatments like vasopressors, inotropes and blood products but was primarily focused on providing fluid resuscitation to obtain and maintain a CVP of 8-12 mm Hg within the first 6 hours of diagnosis recognition. They concluded EGDT provided significantly improved outcomes for patients with severe sepsis and septic shock including improved mortality rates of 30.5% compared to 46.5% for those provided with standard care (P=0.009). They also noted decreased costs from decreased hospital length of stay (LOS) from 18.4±15.0 to 14.6±14.5 days, (P=0.04) [10].
The SCCM, the European Society of Intensive Care Medicine and the International Sepsis Forum, facilitated the Surviving Sepsis Campaign (SSC) in October 2002, an international initiative to increase awareness and improve patient outcomes in severe sepsis. Dellinger, et al., [11] convened to develop the first iteration of the international guidelines for management of severe sepsis and septic shock. Three and six-hour bundle interventions were determined with recommendations based on a modified Delphi grading system; A-E, with A being the highest recommendation. While they incorporated evidence available through the end of 2003, the recommendations were heavily guided by Rivers, et al.’s [10] findings stated above.
Dellinger, et al.’s [11] three-hour bundle required an antibiotic given within the first hour of diagnosis, measure of a lactate level and a 30ml/kg fluid bolus given over half an hour. The six-hour bundle required a remeasure of a lactate if greater than 2.0 and fluid resuscitation to meet a CVP of 8-12 or central venous oxygen saturation (ScVO2) > 70% and the initiation of vasopressors to maintain a MAP > 65mmHg.
Because evidence-based medicine is ever-evolving, Dellinger, et al., [11], would update these clinical practice guidelines in 2008 and again in 2012 [12] with various collaborators and increasing sponsorship from international organizations. EGDT’s focus on aggressive fluid resuscitation and maintaining a CVP of 8-12 was evaluated by various studies between 2013-2014, including the Australasian Resuscitation in Sepsis Evaluation (ARISE), Protocolized Care for Early Septic Shock (ProCESS) and Protocolised Management in Sepsis (ProMISe) studies. Angus et al., [13] performed a systematic review and meta-analysis of EGDT for septic shock including findings from the ARISE, ProCESS and ProMISe studies. They found EGDT compared to usual care or to less invasive alternative hemodynamic resuscitation protocols provided no survival benefit and even increased ICU admission. Their findings did not support the systematic use of EGDT in the management of all patients with septic shock and they did not recommend EGDT for the Surviving Sepsis Campaign guidelines. This opened query into appropriate treatment for septic shock.
In their study, Nguyen, et al. [14] performed a comprehensive committee review of multiple RCTs, meta-analyses, observational and comparison-control studies including ProCESS, ProMISe, and ARISE as well as expert opinion pieces to determine value-based interventions and guidelines in treatment of severe sepsis and septic shock. The guideline committee formed five groups to explore studies of various aspects of sepsis treatment: hemodynamics, infection, adjunctive therapies, metabolic, and ventilation. They applied methodology of Grading of Recommendations Assessment, Development, and Evaluation (GRADE) to determine the quality of evidence and the strength of recommendations selected. Their recommendations are extensive and specific, but foremost, they determined that the use of CVP to guide fluid resuscitation can no longer be justified. Instead they suggest the use of dynamic over static measures in conjunction with passive leg raise (PLR) techniques to determine fluid responsiveness. Further they recommend as a best practice standard that hospitals and systems adopt early sepsis identification and screening.
Rhodes et al., [15] performed a similar committee review to revise and update the 2012 international guidelines. They also incorporated the GRADE methodology to determine the new clinical practice guidelines which echo Nguyen et al.’s [14] findings. Additionally, they proclaim sepsis/septic shock to be a medical emergency requiring immediate treatment and consistent follow-up, re-evaluation and management.
Marik and Bellomo [16] conducted a decision analysis based on the current evidence and contended that recent clinical trials demonstrate that aggressive fluid resuscitation to achieve a CVP > 8mm/Hg does not improve outcomes in patients with sepsis and septic shock. They explain that sepsis is characterized by vasoplegia and venodilation and therefore is not a volume-depleted state. They further argue that aggressive fluid resuscitation carries with it great risk. They quote studies from Brandt, et al., [17] and Rehberg, et al., [18] who found that increased positive fluid balances were directly associated with increased mortality in patients with sepsis and septic shock.
The most enlightening point they made was the deleterious effects of aggressive fluid resuscitation in patients with left ventricular diastolic dysfunction which commonly occurs in patients with hypertension, diabetes, obesity and advanced age. Considering that these healthcare conditions are common in most critically ill patients, they recommend only a 500-ml bolus of Lactated Ringers and do not recommend normal saline (NS) at all in the treatment of sepsis. Marik and Bellomo, [16] also challenge meeting the CVP and ScVO2 measures of EGDT as potentially harmful stating that it is important to remember that the normal CVP is 0-2 mm/Hg. They also found that septic patients who had ScVO2s >90% had higher predictors of death. Quoting Hotchkiss and Karl [19] they even argue that elevated lactates may not necessarily be associated with tissue hypoperfusion.
The measures that Marik and Bellomo [16] agree are consistent with improved outcomes are fluid resuscitation based on fluid responsiveness and early dosing of alpha-1 agonist, Levophed. They believe that fluid responsiveness is most accurately measured by using the PLR while measuring stroke volume (SV). The PLR virtually provides a 250-500 ml bolus. A patient is considered fluid responsive if their SV increases by 10-15% within the first minute of the PLR and they can therefore benefit from a fluid bolus. Those patients who are fluid responsive, receive the bolus and still remain hypotensive will benefit from early use of Levophed.
Marik, Levitov, Young and Andrews [20], performed an electronic chart review of all adult patients admitted to the Sentara Norfolk General Hospital general ICU over an 18-month course. Additional inclusion criteria required the use of bioreactance-coupled PLR maneuver and carotid blood flow data. Bioreactance is a dynamic, or everchanging, measure of cardiac output which can be performed non-invasively. The PLR is performed by lifting the legs 45 degrees passively from the horizontal position which transfers approximately 200-300 ml of blood from the lower limbs toward the heart. If the stroke volume increases at least 10% from the baseline, then the patient is considered fluid responsive, but if it is less than 10% they are not fluid responsive and additional fluids could cause them harm.
Marik, Levitov, Young and Andrews [20], contend that only 50% of unstable patients are fluid responsive. They state overzealous fluid resuscitation is associated with increased mortality, ICU and hospital LOS as well as poorer survival outcomes. Their study revealed that monitoring the hemodynamic response during a PLR was a better determinate for fluid responsiveness in septic patients.
Jakovljevic, Trenell and MacGowan [21], reviewed recent method comparison studies of the use of bioimpedance and bioreactance to estimate cardiac output during fluid challenges. They agree with Marik, Levitov, Young and Andrews’ [20] findings and specify that the bioreactance technique is more robust because it has a higher signal-to-noise ratio. They conclude that a PLR maneuver coupled with the bioreactance NICOM is a simple and accurate method of assessing volume responsiveness in patients with septic shock as well as other critical illness and instability.
In conclusion, a review of data found Sutter Solano least compliant with sepsis bundle guidelines of hemodynamic monitoring. This disparity will be addressed in accordance with the PICOT driven literature review. Sutter Solano Medical Center will onboard NICOM technology in conjunction with PLR to determine fluid responsiveness to adequately treat septic shock in collaboration with eICU care providers.
High-Quality Data Surveillance Evidence
Zhang, et al., [22] state that early detection and resuscitation treatment of sepsis can reduce mortality from 37% to 30.8%. Therefore, the eICU will enhance, institute and manage the high-quality data surveillance screening tool called CMM to better identify and treat septic patients located anywhere in Sutter Solano. While the use of screening tools plays a valuable role in early identification, in the age of EHR, high-quality data surveillance can provide a broader range and scope to screening.
The real-time prospective pilot study of the electronic sepsis surveillance system (ESSV) performed by Brandt et al., [23] ran for 11 days in 2012, involved 477 patients and included a 30-day retrospective trial. The ESSV was 100% sensitive for detecting severe sepsis but only 62.0% specific. They concluded that though this technology was useful in capturing sepsis, they recommended partnering it with surveillance personnel to evaluate the sepsis alerts for false positives thereby improving its specificity. This collaborative partnering could create a valuable tool in the identification of patients with severe sepsis who might otherwise go undiagnosed and untreated.
In their article, Harrison, et al., [24], explain their observational diagnostic performance study that involved all patients age >18 years old admitted to ICU over a three-month period. They reviewed data to develop and test an electronic sepsis screening tool, which they call a sniffer, for capturing delay in recognition and treatment of severe sepsis. They incorporated only the criteria of hypoperfusion/systolic blood pressure (SBP) < 90 mm Hg, SIRS criteria, suspicion of infection, organ dysfunction, Lactate > 2.0 and shock requiring vasopressors in the initial iteration of the sniffer. Each reiteration included more specific data for recognition of end-organ dysfunction and failure: MAP, bilirubin and creatinine levels, Lactate > 4.0, platelets, INR, mechanical ventilation and PaO2/FiO2 ratios, urinary output and GCS score.
Through this study, Harrison, et al., [24] successfully created what they referred to as a severe sepsis ‘sniffer’ which they concluded could accurately identify delay in recognition and treatment. They improved the sniffer’s specificity and sensitivity of 59% and 97% to 80% and 96% through development of the tool’s algorithm. Further they found it could also increase compliance with early therapeutic and diagnostic interventions.
Rhee, et al., [25], performed a comparative retrospective cohort study to determine sensitivity and specificity of electronic data surveillance technology to accurately identify sepsis. They found that more recent studies gained insights from previous ones and therefore have evolved to become more specific and sensitive. The algorithm development and enhancement process undertaken in Harrison’s, et al. [24] study influences the pattern of implementation, enhancement and evolution of the eICU/ICU collaborative project of CMM high-quality sepsis data surveillance technology.
CMM technology was onboarded by the eICU to improve early identification and treatment of sepsis and septic shock at Sutter Solano. Through the eICU personnel’s continuous monitoring and evaluation of these alerts, patient’s lives were saved through early detection and treatment causing their long-term outcomes to improve. Through interdepartmental collaboration, active use and feedback intervals, the CMM technology will continue to be enhanced for appropriate specificity and sensitivity for identification of sepsis. Once accomplished, the enhanced CMM technology can be spread to the other Sutter Health affiliates.
Timeline
The timeline began in May 2016 with the distribution of the “Eliminate Harm Initiative” report from February to April 2016. It was this report that revealed the declining sepsis mortality outcomes. On June 21, 2016, the eICU unit champion (and CNL student) initiated a collaborative with the Sutter Solano Medical Center’s quality improvement team which consisted of their leadership, an educator and an ICU unit champion. While the two collaborative unit champions maintained open communications between the units, Solano’s leadership and educator brought the NICOM equipment and technology to their ICU and ED. Onboarding this equipment was expedited through the NICOM company’s trial programs and educational presentations to staff. On 7/12, Solano’s quality educator placed me in contact with the NICOM company representative so the eICU could also bring educational presentations to its critical care management team. On July 19, 2016, the NICOM representatives came to the eICU to provide educational presentations on the use of NICOM to manage septic shock. By late July, Sutter Solano had partnered with the EHR representatives to launch the inclusion of NICOM orders in the Sepsis/Septic Shock order sets.
On August 4, 2016, Sutter Solano’s Medical Champion facilitated physicians and physician assistants in collaboration to improve access and application of the orders supporting NICOM in EHR. On August 8, 2016, the eICU Director of Nursing launched the pilot-test CMM high-quality data surveillance technology to continuously screen all patients at Sutter Solano Medical center for sepsis. The pilot was initiated for continuous evaluation by the eICU RNs to determine its efficacy and sensitivity to capture sepsis cases. During this time frame, eICU RNs completed a data base noting any unnecessary data collected by the program. Feedback was welcomed and utilized to continually improve the CMM surveillance tool.
On September 19, 2016, the eICU hosted the eICU Journal Club exploration in the latest EBP for fluid responsiveness in sepsis and septic shock. Those in attendance agreed and determined that the PLR in combination with hemodynamic monitoring was the cornerstone for assessing fluid responsiveness in patients with septic shock. Staff agreed to support this initiative throughout its practice.
On September 26, 2016, the eICU launched its upgraded and feedback-enhanced version of the CMM to capture sepsis with increased specificity. Sutter Solano’s leadership announced to their team that the eICU will be will be receiving prompts on the patients that show potential for decompensation. Once the prompt was received, the eICU RN would perform a real-time chart review. All charts requiring intervention would prompt a call for collaborative discussion with the bedside RN. A phone call to a physician or an overhead alert would be implemented if needed.
On September 27, 2016, the collaborating Unit Champions received the ‘go ahead’ for the “President’s Award” eICU/ICU collaborative project. On October 11, 2016, Solano’s leadership made a system-wide announcement of vast improvements in the sepsis mortality rates attributing it to the improved use of sepsis alerts. On November 7, 2016, the NICOM representative came to the eICU and provided three more consecutive educational presentations to most members of the eICU team.
On December 8, 2016, through continued feedback and another technology upgrade, the CMM evolved to screen more rapidly, 600 patients over 15 seconds, and was re-set to run every 30 minutes.
On January 13, 2017, Sutter Solano’s ICU Unit Champion worked as a resource to 1:1 train ICU and ED nurses in the tracking tool’s use in conjunction with NICOM and PLR. Then on January 20, 2017, Solano’s ED Unit Champion facilitated the ‘go live’ with its ED to ICU NICOM trial scorecard (see “NiCOM Trial Scorecard” Table 2) screening tool. This tool tracked care providers for each septic patient as well as records of patients’ arrival time, time the sepsis alert was called, door to initial fluid bolus interval, door to NICOM use interval and door to re-assessment of fluid status/PLR interval. It also prompted the care provider to record whether the patient was fluid responsive upon re-assessment, whether they were hypotensive or required a vasopressor and where the patient was admitted.
Table 2: NiCOM Trial Scorecard
Date:
X Emergency Services ∆ Inpatient Unit
Patient Initials: MRN:
| Goals | Recorded Time | Total Time | Met Goal |
| Arrival time | |||
| Sepsis Alert called Time? | |||
| Door to Fluid Bolus (30ml/Kg | |||
| Door to NICOM ( | |||
| Door to Reassessment of fluid status (< 120 min) PLR/FC? | |||
| Was Pt Fluid Responsive? | |||
| Hypotension Present Y/N | |||
| Vasopressor Started Y/N | |||
| Transfer location? | |||
| Comments or Concerns? |
ED Provider__________ ED RN_________ Hospitalist___________ ICU RN___________
On January 25, 2017, the eICU Unit Champion provided 1:1 education to the eMD to properly order NICOM in EHR because the orders were not readily found. This launched a new cycle of improvement. On January 28, 2017, the various Unit Champions collaborated to provide screen-shots of EHR septic shock order sets to provide easier access to eMDs for off-hour management of these critically ill patients. Then on February 15, 2017, the eICU Medical Director provided all of the eMDs with completed instructions on how to order NICOM in the Septic shock order sets. All eMDs then began ordering NICOM and PLR on all patients admitted to Sutter Solano Medical Center’s ICU.
From February through April, the collaborative teams continued incorporating these process improvement measures and saw the sepsis and septic shock mortality rate continually decrease. The quality data report in April 2017 revealed the effect of the collaborative efforts involved to improved sepsis mortality outcomes at Sutter Solano had dropped the mortality rates from 41.2% to 6.1% (See “Poster Presentation” Figure 3).
Expected Results
The primary expectation was a decrease in mortality rates for septic patients at Sutter Solano Medical Center. Because of the influential reach and success of this project, other leadership in the system are expected to contract to onboard NICOM in effort to improve septic shock mortalities at their affiliates. When the CMM alert system is enhanced and evolved to be robustly specific and sensitive, it will be proposed to introduce it to all of the affiliates in the system. In conclusion sepsis mortality rates can be reduced through implementing the high-quality data surveillance technology, CMM, for early identification and treatment of sepsis. Further, the use of NICOM in conjunction with PLR for determining fluid responsiveness is the most current EBP recommended guideline for fluid resuscitation in sepsis and septic shock. The system could conclude to use NICOM and CMM high-quality data surveillance throughout all the affiliate hospitals for improved quality outcomes for septic patients.
Nursing Relevance
The evaluation of EGDT for fluid resuscitation has been under scrutiny as a Surviving Sepsis Campaign guideline since 2012 for its focus on CVP measures to determine fluid resuscitation. Nursing needs to recognize that CVP is no longer recommended or accepted as a measure of hemodynamic stability. The latest EBP supports NICOM in conjunction with PLR as a foundational guideline for fluid resuscitation.
It could be speculated that the next Surviving Sepsis Guidelines will incorporate NICOM in conjunction with a PLR to determine fluid responsiveness and guide fluid resuscitation in septic patients. Further the CVP will likely no longer be employed as a 6-hour bundle measure along with its accompanying ScVO2 measure. Rather, the guidelines may be compelled to require NICOM/PLR and a focused physical exam that can be performed by nursing with physician countersignature to meet 6-hour bundle requirements. Lastly, the eICU/ICU collaborative to improve sepsis mortality is a partnership worth incorporating throughout healthcare as a critical care quality improvement measure.
The value of nursing assessment and evaluation of the septic patient to ensure proper standard of care cannot be overstated. Enhanced high quality data surveillance technology can offer benefit to early recognition of sepsis appreciating that most important treatment in sepsis and septic shock is the first antibiotic which must be given within one hour of recognition. Further, providing adequate fluid resuscitation and vasopressor rescue and support of the cardiovascular system is the next treatment to prioritize. Care providers must recognize that a CVP >8 mmHg is not an indicator of fluid responsiveness and can in fact cause lung and kidney injury. Most importantly, the goal of sepsis treatment is optimal tissue perfusion rather than fluid resuscitation. It is important to remember in the absence of hemodynamic monitoring that repeat lactate measures are emphasized as adequate indicators of tissue reperfusion [26].
Conclusions
This project contains many of the qualities of a high-performing clinical microsystem as described by the Institute for Healthcare Improvement [27]. The Institute for Healthcare Improvement (IHI) states for a unit to produce synergistic outcomes, it must possess qualities such as leadership, being patient-focused and staff attractive, promoting process improvement, incorporating macro-system support of its microsystem, optimization of information and information technology and being performance driven [28]. This project contains within its processes all of these characteristics.
First, the project requires microsystem leadership which is supported by Sutter’s eICU Director of Nursing and the Sutter Solano leadership. The project focuses on patients by improving outcomes for septic patients and incorporates an interdependent care team. The aspect of the project that brings most of these characteristics together is the implementation of the CMM sepsis alert. It attracts staff from all areas of the hospital to address the patient’s needs. The alert activates lab technicians, radiologists, physicians and intensivists, nurses, pharmacists and respiratory therapists to work together seamlessly to provide best practice implementation of interventions in a timely manner. The CMM sepsis alert depends on information provided by nursing documentation and requires information technology to be activated within the EHR and communicated to the eICU database. The project created process improvement as all patients who arrive via the ED at Sutter Solano medical Center are now electronically screened for sepsis in effort to improve early recognition and treatment. This reflects how the microsystem supports the macro-system changes. The PDSA cycles already implemented correlate to improved outcomes which is an improved performance result.
The sustainability of this project will be integrated over the course of repeated educational presentations regarding NICOM and PLR by representatives and unit champions. In conjunction with local chapter AACN, physician speakers will present this information to many accessible locations in the system’s vicinity. In the eICU, the Journal Club will continue its explorations in the latest evidence as it is published. The CMM technology has continued support from staff, leadership and pharmacy administration. At Sutter Solano, the NICOM/PLR technology has been fully adopted and is supported by EHR and a dedicated quality improvement team. The project’s initiative interventions are easily adoptable at this stage and are already integrated into workflow in both units and throughout the system as presently implemented. Inspired by the improved outcomes at Sutter Solano Medical Center, other Sutter ICUs are on-boarding the NICOM technology and considering the CMM technology.
References
- Afrefian H, Heublein S, Scherag A, Brunkhorst FM, Younis MZ, et al. (2017) Hospital-related cost of sepsis: A systematic review. Journal of Infection 74: 107-117.
- Society of Critical Care Medicine (2016) Critical Care Statistics. Retrieved from: http://www.sccm.org/Communications/Pages/CriticalCareStats.aspx
- American Association of Colleges of Nursing (2013) Competencies and curricular expectations for clinical nurse leader education and practice. Retrieved from http://www.aacn.nche.edu/cnl/CNL-Competencies-October-2013.pdf (Links to an external site.)
- Klompas M, Rhee C (2016) We Need Better Tools for Sepsis Surveillance. Crit Care Med 44: 1441-1442. [crossref]
- American Association of Colleges of Nursing (2007) White paper on the education and role of the Clinical Nurse Leader. Retrieved from: http://www.aacn.nche.edu/Publications/WhitePapers/CNL2-07.pdf
- Gaieski DF, Edwards JM, Kallan MJ, Carr BG (2013) Benchmarking the incidence and mortality of severe sepsis in the United States. Crit Care Med 41: 1167-1174. [crossref]
- Massoud MR, Nielsen GA, Nolan K, Nolan T, Schall MW, et al. (2006) A framework for spread: From local improvements to system-wide change. IHI Innovation Series white paper. Cambridge, Massachusetts: Institute for Healthcare Improvement (Available on www.IHI.org).
- Kotter (1996) Kotter's 8-step change model: Implementing change powerfully and successfully. Retrieved from: http://www.strategies-for-managing-change.com/support-files/kotterchangemodel.pdf
- Marx G, Scheeren TWL (2016) Advanced hemodynamic monitoring in the critically ill patient: Nice to have or need to treat? Journal of Clinical Monitoring and Computing 30: 507-508.
- Rivers E, Nguyen B, Havstad S, Ressler J, Muzzin A, et al. (2001) Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Engl J Med 345: 1368-1377. [crossref]
- Dellinger RP, Carlet JM, Masur H, Gerlach H, Calandra T, et al. (2004) Surviving sepsis campaign for the management of severe sepsis and septic shock. Intensive Care Medicine 30: 536-555.
- Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, et al. (2013) Surviving sepsis campaign: International guidelines for management of severe sepsis and septic shock, 2012. Intensive Care Medicine 39: 165-228.
- Angus DC, Barnato AE, Bell D, Bellomo R, Chong CR, et al. (2015) A systematic review and meta-analysis of early goal-directed therapy for septic shock: the ARISE, ProCESS and ProMISe Investigators. Intensive Care Medicine 41:1549–1560.
- Nguyen HB, Jaehne AK, Jayaprakash N, Semler MW, Hegab S, et al. (2016) Early goal-directed therapy in severe sepsis and septic shock: insights and comparisons to ProCESS, ProMISe, and ARISE; Critical Care 20: 1-16.
- Rhodes A, Evans LE, Alhazzani W, Levy MM, Antonelli M, et al. (2017) Surviving sepsis campaign: International guidelines for management of sepsis and septic shock: 2016. Critical Care Medicine 45: 486-552.
- Marik P, Bellomo R (2016) A rational approach to fluid therapy in sepsis. Br J Anaesth 116: 339-349. [crossref]
- Brandt S, Regueira T, Bracht H, Porta F, Djafarzadeh S, et al. (2009) Effect of fluid resuscitation on mortality and organ function in experimental sepsis models. Crit Care 13: R186. [crossref]
- Rehberg S, Yamamoto Y, Sousse L, Bartha E, Jonkam C, et al. (2012) Selective V(1a) agonism attenuates vascular dysfunction and fluid accumulation in ovine severe sepsis. Am J Physiol Heart Circ Physiol 303: H1245-1254. [crossref]
- Hotchkiss RS, Karl IE (1992) Reevaluation of the role of cellular hypoxia and bioenergetic failure in sepsis. JAMA 267: 1503-1510. [crossref]
- Marik PE, Levitov A, Young A, Andrews L (2016) The use of bioreactance and carotid doppler to determine volume responsiveness and blood flow redistribution following passive leg raising in hemodynamically unstable patients.
- Jakovljevic DG, Trenell MI, MacGowan GA (2014) Bioimpedance and bioreactance methods for monitoring cardiac output. Best Practice & Research Clinical Anaesthesiology 28: 381-394
- Zhang Z, Smischney NJ, Zhang H, Van Poucke S, Tsirigotis P, et al. (2016) AME evidence series 001—The Society for Translational Medicine: Clinical practice guidelines for diagnosis and early identification of sepsis in the hospital. Journal of Thoracic Disease 8: p 2654-2665.
- Brandt BN, Gartner AB, Moncure M, Cannon CM, Carlton E, et al. (2015) Identifying severe sepsis via electronic surveillance. American Journal of Medical Quality 30: 559-565.
- Harrison AM, Thongprayoon C, Kashyap R, Chute CG, Gajic O, et al. (2015) Developing the surveillance algorithm for detection of failure to recognize and treat severe sepsis. Mayo Foundation for Medical Education and research 90: 166-175.
- Rhee C, Kadri S, Huang SS, Murphy MV, Li L, et al. (2016) ‘Objective sepsis surveillance using electronic clinical data’. Infection Control & Hospital Epidemiology 37: pp. 163-171.
- Hernandez G, Pedreros C, Veas E, Bruhn A, Romero C, et al. (2012) Evolution of peripheral vs metabolic perfusion parameters during septic shock resuscitation. A clinical-physiologic study. Journal of Critical Care 27: 283-288.
- Institute for Healthcare Improvement (IHI) (2017) Improving health and healthcare worldwide: Clinical microsystem assessment tool. Retrieved from: http://www.ihi.org/resources/Pages/Tools/ClinicalMicrosystemAssessmentTool.aspx
- Marik PE (2016) Fluid responsiveness and the six guiding principles of fluid resuscitation. Critical Care Medicine (XX)XXX DOI: 10.1097/CCM.0000000000001483
